 Let’s say you’re waiting for your mammogram results, and you get a callback. What next?
Let’s say you’re waiting for your mammogram results, and you get a callback. What next?
First, stay calm.
I got the dreaded callback, too.
As a follow up to my post about my first mammogram, here are 10 things I learned, in the hopes that they might help you, too.
1. What’s wrong with me!?
Don’t worry if by the end of the call, you still don’t know. I was asked to come back in because “the results were inconclusive.” Calls of this sort are purposefully vague. That’s because “inconclusive” could mean anything from a shadow on the film to something completely benign to full-on breast cancer. The radiologist can’t give you that prediction over the phone. They don’t know for sure (either way), and they don’t want to be responsible for setting up false hopes or expectations.
Just try to absorb this message for what it is: completely devoid of information. Which leads me to my next point …
2. Schedule a follow up ASAP.
Why wait, thus increasing your stress? That will only make things worse. Get back into that office, the sooner the better.
And this is important: When you’re scheduling your appointment make sure there will be someone on hand to review your results that day. You don’t want to wait another week for the results, which could include another check, another appointment, another wait for results, etc.
In my case, the scan reviewer would be in the office Tuesday and Friday that week, and both of those days were already booked. It was a Wednesday, and I was leaving for an 8-day vacation on Friday night. When I told the scheduler this, she double booked a Friday appointment for me, so I wouldn’t have to wait that long.
Even if you have to lie and say you’re leaving the country to save orphaned kangaroos in Australia next week, do it. You need information, and you need it now. Be. Aggressive. Be be aggressive.

3. False alarms
No one knows for sure how many women get false-alarm callbacks, but they do know the number is very high. Why? Advances in digital imagining now show every little thing (worrisome or not), particularly this culprit …
4. Calcifications
There are two different kinds (macro and micro). Both are calcium deposits in breast tissue that appear as white specks or spots on a mammogram. They’re so small, you usually can’t feel them.
The macro kind is rarely associated with cancer. About 50% of women over 50 have them (10% for those us under 50).
If you’re getting a call, it’s likely due to microcalcifications. According to the Mayo site:
Breast calcifications can be seen on mammograms performed in most women.
More good news:
It’s estimated that 80% of breast tissue microcalcifications are noncancerous (benign).
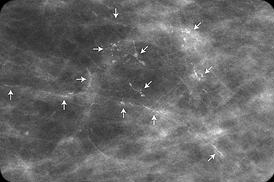
What they saw on my scans was a splattering of salt-grain-sized microcalcifications on my left breast. In such cases, they need to take a closer look to make sure there aren’t any red-flag patterns, like tight clusters or irregular shapes.
5. “Don’t cook your babies.”
No joke, that was a direct quote from my OBGYN when we were trying to get pregnant with my daughter. She was referring to hot tubs. The same holds true with X-rays, but of course, much more so.
If there’s any chance you might be (or want to be) pregnant soon, you’ll want to (1) schedule your appointment during your period and (2) ask for the special X-ray protecting belt. It’s very sexy—perfect for making babies.

6. It’s going to take longer this time.
Allow for at least twice as much time as your previous appointment. I made the mistake of paying too little for street parking and had to sneak out to put more money in the meter while I awaited my results.
Better yet, clear your schedule for the whole day, and go in the morning. Then, best case scenario, you’ll have some much-deserved me time afterward. Worst case scenario, you might need some me time then, too. But let’s stay positive, okay? Remember what I said about stress.
7. First stop: X-ray machine.
They took about 2-3 times as many “pictures” my second time. Maybe that won’t be the case for you, but if it is, that’s totally normal. Since this is a callback, they want to check you out, over, under, and sideways. This is a good thing. The more pictures, the more confidant you and your doctor can be about the results.
8. Possible second stop: ultrasound.
Fresh in from feeding the parking meter, I returned to the waiting area and mindlessly leafed through old Cosmopolitans. You know how The Little Engine That Could repeats, “I think I can, I think I can”? I had a similar chugging happening in my brain. “It’s probably not. It’s probably not … ”
I was trying really REALLY hard to keep that train on course. I was doing a damn good job of it, too, until …
The nurse came out, put her hand on my shoulder, and regretfully informed me, “We’re going to need to do an ultrasound.” I didn’t know what that meant, but judging by her tone and body language, I didn’t like it.
So they took me into a room, put some jelly on my breast, and poked around with a wand attached to a computer. (Trust me. It’s not as erotic as it may sound. Not even close.) The technician explained that they had seen one larger white spot in my X-rays. They were hopeful that it was just a lymph node, but needed an ultrasound to confirm it. Apparently liquid shows up white in X-rays and black in ultrasounds, so they were looking for a black spot in the same location as the white spot on the previous scan.

It took awhile, and she couldn’t find it. She had to call in the doctor. I had been doing so well until then, but all the sudden I couldn’t hold back the surge of fear … or a few tears. The technician either didn’t notice or kindly ignored them. I’m sure that’s a hazard they’re used to in their line of work.
9. Possible third step: biopsy.
I didn’t get to this step because the doctor finally found what he wanted to see: the black spot of that lymph node. However, he said that if any of my calcifications had been large enough, they would’ve done a biopsy. Apparently they use a long, thin, hollow needle to remove some of the questionable tissue and make sure it’s okay.
I have to admit, it sounds painful; however, I didn’t experience it, so I can’t say. If your doctor has requested a biopsy, here’s some more info about it.
10. Keep an eye on it.
Even if everything is okay, they’ll likely ask you to come back six months or a year later. My radiologist told me there was “a less than 2% chance” that my calcifications were cancerous, based on what he saw (or didn’t see) and my family history. I’m going back in six months so they can see if anything has changed.
The name of the game is consistency. They want to make sure those specks aren’t moving, growing, or grouping. Breast cancer experts also recommend you go to the same imaging center for follow ups. That way, they’re using the same equipment and views, to get the best possible comparisons.
And I leave you with this …
Please please PLEASE tell every woman you know about the importance of early detection. If caught early, there’s a 98% survival rate. But sadly, 30% of women are diagnosed after their breast cancer has spread. We can help fix this by demanding earlier scans for earlier detection. Even with the history of my grandmother’s premenopausal breast cancer, I had to push through the red tape to get checked at age 36, four years before the recommended age of 40. That’s why I was so flabbergasted when the ultrasound tech said, “If only we had scans of you from three years ago, then we would know for sure.” So if I had waited until 40, as many insurance companies and doctors require, then I might not have know “for sure” until age 43? That’s pushing it in my book. I love life too much. I’m not willing to gamble it like that. No one should expect you (or your wives, sisters, mothers, daughters, and friends) to either.

If it’s not a pretty sight (ie, if they suspect it might be cancerous) you will most likely get both an ultrasound and a biopsy. The ultrasound doesn’t hurt at all, of course; my needle biopsy wasn’t terribly painful, really no worse than the average mammogram.
In my case the doctors were able to tell me immediately that they thought the mass looked malignant; the biopsy was just to confirm.
I then had a stereoscopic biopsy of other areas of calcification in my breast, and that was really painful and shocky – but they weren’t cancerous!
And the cancer hadn’t spread to my nodes – I found a mass on a Saturday, and by the end of the week was in the system. Early detection saves lives.
Thaanks great blog post